‘None of us will ever be the same’: Survivors of 2017 Tubbs Fire face long-term trauma
Robert “Priest” Morgan hasn’t slept without a cocktail of pills since the night he says God kicked him in the head to wake him up – the night he opened the front door of his Santa Rosa mobile home to see a fire engine, a few people running up and down Sahara Street and screaming.
“The sky looked like the Fourth of July,” he said. “The entire park except for my street was an inferno.”
It wasn’t Independence Day – it was Oct. 9, 2017, and the Tubbs Fire had broken the Santa Rosa city limits.
A wiry, Harley-riding jack-of-all-trades – he’d spent a year and a half with the Diamond Springs fire brigade – Morgan grabbed a hose firefighters passed him through his fence and helped them battle the blaze back from the 44 last standing homes in Journey’s End mobile home park.
But last November, when smoke from the Camp Fire blew into Santa Rosa from 150 miles away, Morgan got into his car and bolted.
He’d considered himself a tough man – and looked the part, too, with slicked-back hair, a sleeve of tattoos and a thick, neat mustache – but the Tubbs Fire broke him.
“I went full-blown PTSD, I panicked – I ran as fast and as far as I could. And the only thing I could think of was to go someplace where there were no fires.”
He roamed around Northern California, frantic and aimless, but the fire was inescapable, the omnipresent subject of gas station conversations and TV newsreels.
Finally, he headed to San Francisco International Airport and bought a ticket to Minneapolis, where winter was already entrenched. He checked himself into a hotel, holed up indoors by day and wandered around in freezing cold weather by night.
He now lives in Wisconsin with his ex-wife. “(The counselor) I’m working with said, ‘You’ve been hit so hard by this, you go back where fires happen on a regular basis and it’s gonna happen all over again,” he said.
“I consider me leaving California a medical emergency.”
The ‘new normal’
Since the Tubbs Fire consumed 5,600 structures and took 22 lives nearly two years ago, disastrous wildfires have become California’s “new normal,” as then-Gov. Jerry Brown said last August. But survivors of the fire are coming to terms with their own new normal: Mental landscapes troubled by the long wake of trauma.
Each of California’s increasingly intense fire seasons will leave a growing population traumatized, the physical damage to their homes and workplaces mirrored by internal disarray and emotional distress, mental health experts say.
But many survivors do not experience – or rather, recognize – the worst effects of trauma until long after the event, specialists and social workers agree.
As the two-year anniversary of the Tubbs Fire nears, mental health providers are buckling in for a surge in demand.
Not only will the anniversary act as an emotional choke point, it also marks the end of insurance payouts. As Bay Area home prices continue to rise, displaced residents still in limbo will be left to shoulder compounded housing costs, sometimes for more than one property: A rental and a new home under construction; a rental and an old mortgage on an unlivable home that the bank won’t cancel.
Megan Carlock, a Santa Rosa-based trauma specialist who worked for California HOPE, a federally funded post-disaster counseling provider, said the delay in seeking treatment owes to survivors’ tendency to put mental recovery after material recovery, or to assume the former follows naturally from the latter. California HOPE sought people out at shelters and rentals rather than waiting for them to recognize their symptoms, prioritize their mental health and seek aid, she said.
“When life gets stressful, people focus on doing,” she said. “‘If I just do this and get this handled, all these things are going to go away. The stress is about the rebuild.’ When in fact before the rebuild even hit, you had this tremendous impact to your nervous system that you’re still recovering from.”
Only after the period of pressing logistics passed did greater numbers of survivors begin to register the toll that disaster and loss took on their mental health: Providers saw upticks in calls for aid at the fire’s six-month and one-year anniversaries, as well as during major nearby fires, like the Mendocino Complex Fire in late July last year, and the Camp Fire in November.
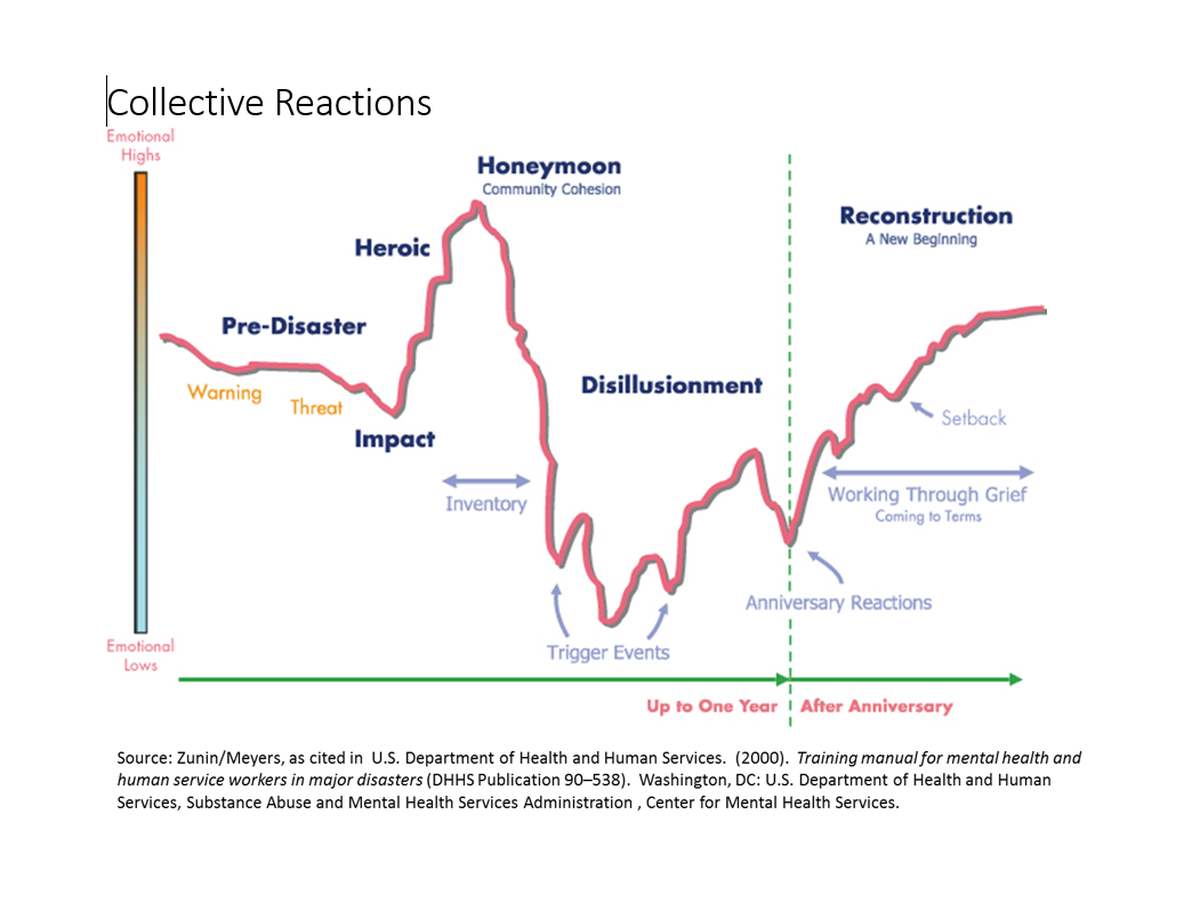
“I’ve talked to people who say, ‘It’s been a year, why am I having a hard time?’ Well, the first year you’re in shock, so the second year really is often harder,” concurred Carlock’s friend and Santa Rosa resident Susan Dunn. Dunn is also a trauma specialist, and runs support groups for the National Alliance of Mental Illness.
“And when people don’t know that, they start to turn it against themselves: ‘There’s something wrong with me!’ No, there’s nothing wrong with you. You have a nervous system, it has a path of healing, and there are some things you can do to help it.”
Path forward for treatment
Now Cal HOPE has come to the end of its funding from the Federal Emergency Management Agency, having served nearly 100,000 people since October 2017. Wheelright said the organization has passed the baton to the foundation-funded Wildfire Mental Health Collaborative and Sonoma County Resilience Collaborative.
Both collaboratives are flexible and expansive, bringing national expertise to local communities in a loop that benefits both: Experts are figuring out how best to deal with the increasingly urgent issue of post-disaster trauma so future disaster-struck communities won’t have to reinvent the wheel, and fire-affected neighborhoods are receiving the best possible care at close quarters.
The Wildfire Mental Health Collaborative offers individual and group counseling in Skills for Psychological Recovery, trauma-informed yoga and a digital health app called Sonoma Rises, all of which are free, while the Sonoma County Resilience Collaborative is training community members – medical professionals and laypeople alike – in an evidence-based self-care program called Mind-Body Medicine.
Skills for Psychological Recovery and Mind-Body Medicine are both highly practical, aimed not at rooting out age-old mental illness through in-depth, individual counseling but at efficiently cultivating resilience, both individual and communal. They serve a wider range of people, facing a wider range of symptoms, than do traditional PTSD treatments.
In fact, the diagnosis of PTSD – denoting the presence of intrusive memories, flashbacks, hypervigilance and negative alterations in cognition and mood – has lost some stead among trauma specialists and mental health advocates.
“A lot of people argue that clinical diagnoses are arbitrary,” said Dr. Adrienne Heinz, clinical research psychologist at the National Center for PTSD. Instead, specialists favor the term post-traumatic stress reactions – or just plain post-traumatic stress – which they say is less stigmatizing and more utilitarian. Rather than checking for a particular pathology, Heinz assesses patients’ ability to “live the life they want to live.”
Paths to recovery are paved by support systems, experts say: Individuals can’t be healthy without healthy communities, and communities can’t be healthy without healthy individuals.
Survivors find great comfort in the solidarity unique among people who have undergone the same series of traumatic experiences.
“It’s like the redwood forests. Their roots interconnect to hold each other up,” Wheelwright said. “That’s how those trees get so tall.”
“We all have our own work to do,” Dunn said, “but our fate is interdependent.”
A community dispersed
Morgan turned 64 on July 12 in Wisconsin, far from his family and friends. In the morning, he got a “birthday haircut.” Later, he took a therapeutic ride on his beloved Harley-Davidson, which his family shipped to him from California.
Over and over he returns to an image, “tattooed” on his brain, of Martha Sue Sinnott, a disabled elderly woman whom he rescued from her flame-enveloped home. “Her mouth was closed, but her eyes were screaming a deafening scream.”
The 44 homes he saved were swiftly red-tagged by the city government. Kendall Jarvis, disaster relief attorney for Legal Aid of Sonoma County, said insurance companies used that as a loophole to evade insurance claims: The homes were lost due to government action, not a natural disaster, they said, and they didn’t cover such losses.
The residents were left without homes or compensation, a state of affairs that torments Morgan: “I tell people it’s my greatest achievement and my deepest regret all at the same time.”
By November 2018, conceding to the advice of family members, he’d enrolled in counseling and completed three sessions. But his nascent recovery was cut short when Camp Fire smoke drove him from California.
Now, Kaiser Permanente considers him out of plan, so his sister pays for his counseling out of pocket. In March he was told he’d be dropped from the health plan if he didn’t return to California within six months.
Tarek Salaway, senior vice-president and area manager for Kaiser Permanente’s Marin-Sonoma service area, said, “We recognize and thank Mr. Morgan for his many contributions to the community during and after the North Bay fires. We are sympathetic to his situation, and to that of so many in the North Bay who remain affected by the devastating fires in 2017. Kaiser Permanente continues to serve as a committed partner to our community ... We value Mr. Morgan as a Kaiser Permanente member and are committed to working with him to help meet his needs and resolve any concerns.”
The other residents of Journey’s End are dispersed across homes and rental apartments in and out of state. Burbank Housing is developing the former mobile home park into a low-income apartment building that former residents say they can’t afford. The scarcity of low-income housing, bad before and worse after the fire, has pushed them farther afield and apart.
Dispersal has hurt communities of seniors in particular, who aren’t always wired up on social media, a crucial means of post-fire connection for younger generations. Neither do seniors always have the earning power or energy to mobilize for themselves and their communities – although some fiery Journey’s End residents organized a protest against post-disaster housing injustice under the slogan “Senior Lives Matter.”
Morgan was one of Journey’s End’s younger inhabitants, and losing him to his trauma-induced move was a further blow to community cohesion.
Shirlene Gilman and Dorothy Hughes, two of Morgan’s friends, concurred he wasn’t the same – but said they weren’t, either.
“I lost my life that night,” Gilman said. “I’m talking to you right now but I lost my life that night.”
Like Priest, Gilman is prone to tears and triggered by wind and fire. She was weeks away from homelessness when a Catholic charity relocated her to her current home in the Santa Rosa Junior College neighborhood. It’s only an eight-minute drive away from her former Journey’s End residence, but her tight-knit support network of old – “We were our own little family,” she said – has dissolved.
For a time, she and several other former Journey’s End residents met weekly on Monday to support each other through the cavalcade of difficulties they share: monthly incomes of $1,200, housing insecurity, physical ailments resulting from age and post-traumatic stress.
But the meetings recently ended, and Gilman is at the end of her tether. Bereft of material proof of the life she has lived and skeptical of the American political future – “My grandkids are going to be fighting over water!” – she pronounced, “I’m going to die now and get the hell out of here, because I don’t like where we’re going.”
Death was on Dorothy Hughes’ mind, too: “It’s like they’re waiting for us to die so they don’t have to deal with us anymore,” she said. “Quite frankly I have lost hope.”
Debbie Mason, CEO of the Sonoma County Healthcare Foundation, said she has personally handed fliers for the Foundation-funded Wildfire Mental Health Collaborative to Journey’s End residents. But the post-disaster dispersal means that resources are difficult to distribute and outreach happens person by person.
Neither Gilman nor Hughes had heard about or received post-disaster counseling, although they both described hampered mental landscapes. “I’m so stressed out I can’t think,” Hughes said.
“None of us will ever be the same people we were,” Gilman said.
How can you get help?
Resources are available for fire survivors in the Santa Rosa area.
- Call or text (866) 960-6264 to get started with free individual counseling, or email DMason@healthcarefoundation.net to schedule a private group session.
- You can also attend free, public support groups for wildfire survivors, or try free yoga for stress reduction and trauma resolution – a physical extension of intentional breathing. A full list of resources is available on the Healthcare Foundation’s website: https://healthcarefoundation.net/fire_recovery/.
- The Sonoma County Resilience Collaborative is setting up group sessions; a limited calendar is available on the Santa Rosa Community Health website. For information about when a group might be set up near you, contact program coordinator Gricelda Correa at griceldac@srhealth.org or (707) 547-2220, ext. 3773.
This story was originally published August 2, 2019 at 5:00 AM with the headline "‘None of us will ever be the same’: Survivors of 2017 Tubbs Fire face long-term trauma."