California’s evolving debate over dry needling safety and training | Opinion
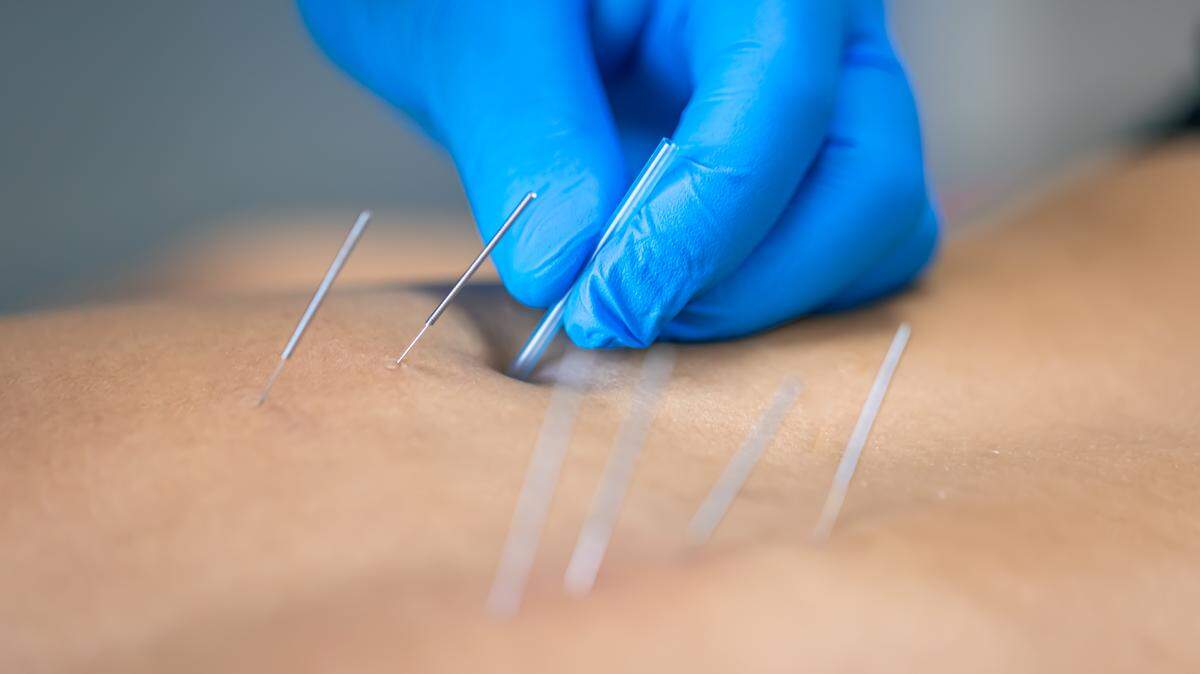
In recent years, a quasi-therapeutic practice known as dry needling has gained visibility in physical therapy and sports medicine settings. In this procedure, a physical therapist inserts thin needles through the skin into muscles or other soft tissues, often with the stated goal of relieving pain, releasing trigger points or improving movement — a practice that supporters frame as a distinct Western clinical technique, but critics say is simply acupuncture by another name.
The problem is that there is no formal training for dry needling, unlike acupuncture, which takes years of training.
Now, a bill moving through the California Legislature — Assembly Bill 2497 — would allow physical therapists to administer dry needling without additional training.
On April 21, nearly 200 people gathered in the rain outside a legislative hearing on AB 2497, authored by Assemblymember Natasha Johnson, R-Corona. Inside the Assembly Business and Professions Committee, they voiced concerns about a bill that would allow physical therapists to perform invasive needling procedures without requiring the same level of training as licensed acupuncturists. The measure advanced narrowly, with a vote of 10–8-1.
To understand the stakes, it is important to understand what California law already states: Under existing law, acupuncture is not loosely defined. It is specifically recognized as the stimulation of points on or near the surface of the body by inserting needles to prevent or modify the perception of pain, or to normalize physiological functions. The definition also explicitly includes related techniques, such as electroacupuncture, cupping and moxibustion.
In other words, the act of inserting needles into the body for therapeutic purposes is not incidental — it is the very core of what the state defines as acupuncture.
Whether called acupuncture or dry needling, the physical act is fundamentally the same: penetrating the skin with a needle to affect underlying tissue. And with that act, comes anatomical risk.
When Pittsburgh Steelers edge rusher T.J. Watt — the 2021 NFL Defensive Player of the Year — suffered a collapsed lung from a dry needling treatment last December, it drew attention far beyond professional football. Watt’s situation was a sobering reminder that any procedures involving needles are not risk-free.
A collapsed lung, or pneumothorax, is one of the known complications when needling is performed near the chest. Though rare, it is well documented. Avoiding such outcomes requires not only caution, but deep anatomical knowledge, clinical training and supervised experience.
That is why California has long required licensed acupuncturists to complete years of formal education and clinical training before performing these procedures. These standards exist because needling is an invasive intervention.
AB 2497 raises a difficult question: Should the state allow similar procedures to be performed under a different name, but without equivalent training requirements?
Supporters argue that expanding access could improve efficiency and reduce barriers to care. But cases like Watt’s highlight a critical reality: when training does not match the level of risk, even routine procedures can lead to serious consequences.
This is not about professional titles. The human body does not distinguish between “acupuncture” and “dry needling.” It responds only to precision — or error.
As AB 2497 moves forward, lawmakers face a responsibility that extends beyond scope-of-practice debates. They must decide whether expanding access should come with an equal commitment to safety — and whether redefining procedures risks undermining the very standards designed to protect patients.
When it comes to inserting needles into the human body, definitions are not just words, they are safeguards.
Le Jiang is a licensed acupuncturist, a doctor of acupuncture and oriental medicine and a member of the American Association of Chinese Medicine and Acupuncture based in Sacramento.