Four years and $300 million later, what’s California’s dialysis ballot proposition really about?
Service Employees International Union-United Healthcare Workers West, or SEIU-UHW, evolved into one of California’s fiercest political players in 2018 when it bankrolled a ballot initiative to more stringently regulate the state’s for-profit dialysis industry.
California voters rejected it by a wide margin, and did so again in 2020. Both sides spent a total of nearly $300 million for what union leaders called a fight for reform, and what the industry says is a strategy of economic attrition to force it to the bargaining table.
In November, UHW will return to the ballot, this time in the form of Proposition 29.
A “yes” vote would support changing regulations to require a physician, physician assistant or nurse practitioner to monitor patients’ dialysis treatments. It would also mandate clinics to disclose the names of physicians with an ownership interest of more than 5%; to report dialysis-related infections to the California Department of Public Health, and to obtain written consent before closing a clinic or reducing patient services.
A “no” vote would maintain the status quo.
Once again, it faces opposition from the state’s leading dialysis providers, DaVita and Fresnius, the California Medical Association, the state’s Dialysis Council and the California Chamber of Commerce.
Here are answers to some questions about Proposition 29.
WHAT’S DIALYSIS?
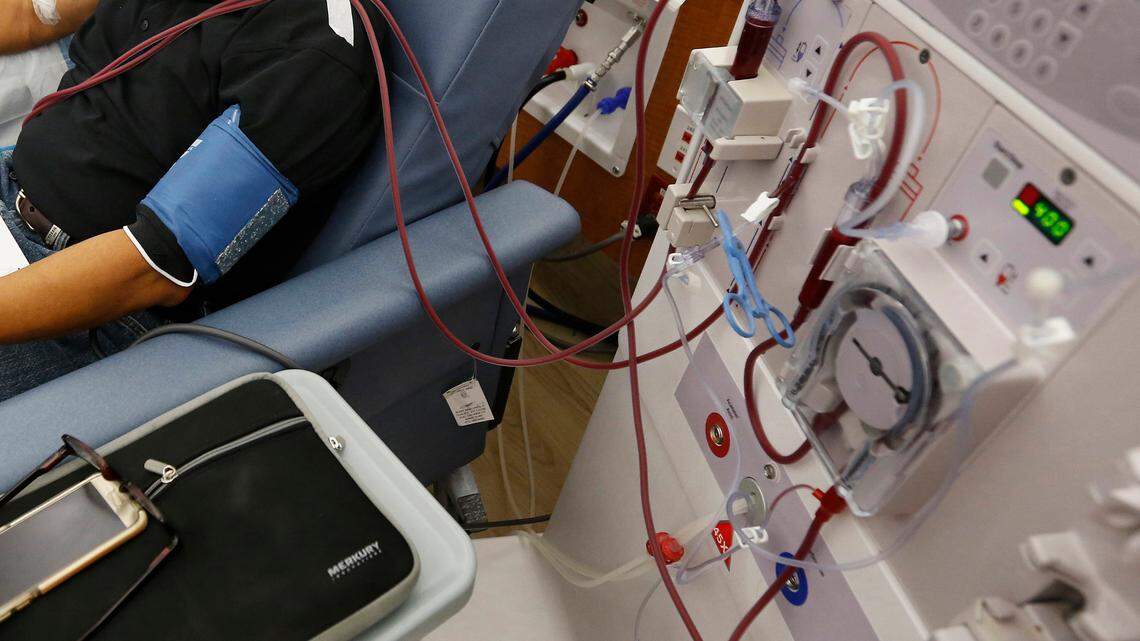
It’s a medical procedure for people whose diseased kidneys are no longer able to remove waste and other chemicals from the bloodstream. Dialysis involves removing their blood and filtering it through a machine that cleans and returns it.
In most cases, patients receive treatment around three times a week, with each session lasting roughly four hours. California has about 650 licensed dialysis clinics, which serve an average of 80,000 patients a month.
WHO OPERATES THE CLINICS?
DaVita and Fresnius, two big national companies, dominate the industry in California, operating 75% of all clinics, according to the state Legislative Analyst’s Office.
The facilities are regulated by the California Department of Public Health, which licenses and certifies them on behalf of the federal government so that they can accept Medicare and Medi-Cal payments.
According to federal regulations, a medical doctor must be present at clinics during treatment, but such a role is listed as one-quarter of a full time position. Clinics are required to report dialysis-related infection data to a national network.
WHAT’S THE CASE FOR MORE REGULATION OF THE DIALYSIS INDUSTRY?
California dialysis clinics collect annual revenues of $3.5 billion, most of it coming from Medicare, Medi-Cal and private insurance. Advocates say the industry overcharges patients and under-delivers results.
Recent research has pointed to worsening outcomes for dialysis patients in the U.S — especially as the industry consolidates under the control of several companies.
“As large, for-profit dialysis chains acquired more than 1,200 smaller providers across the U.S. from 1998 to 2010, they cut skilled medical staff, increased patient volumes, altered drug regimens and adopted other practices that hurt patient health,” a group of researchers at Duke University found in 2019.
The Duke study said that after a dialysis clinic was acquired by a for-profit chain — like DaVita or Fresnius — a patient was over 4% more likely to be hospitalized in any given month. It also found that survival rates post-acquisition fell by up to 2.9%. Patients were 8.5% less likely to receive a kidney transplant or be placed on a transplant waiting list during their first year of dialysis.
In California, where the industry is remarkably consolidated, advocates have continued to sound the alarm.
“These dialysis initiatives have really been about regulating an industry that has a duopoly, high profit rates and well-documented patient safety concerns,” said Laurel Lucia, director of the Health Care program at the UC Berkeley Labor Center.
WHAT DOES THE INDUSTRY SAY?
Forcing clinics to hire more physicians would cost too much. A fiscal report from the state estimates that the measure could raise health care costs for state and local governments “by low tens of millions of dollars annually.”
The policy, according to the report, would boost clinics’ costs by “several hundred thousand dollars” annually. But it also points out that the impact of the higher costs could be softened by distributing them across all clinics.
Kathy Fairbanks, spokesperson for the No on Prop 29 campaign, said the Duke study is based on old Centers for Medicare & Medicaid Services data from 1998 to 2010 and “doesn’t give insight into what’s going on in California at all.”
She added that newer CMS data, from as recently as 2021, shows California ranking above the national average in both quality of care and patient satisfaction.
CMS, however, does not do state rankings of dialysis. The California ranking was derived by dialysis providers using CMS data. Fairbanks said.
THE INDUSTRY SAYS PROP. 29 IS AN ORGANIZING TACTIC. IS THAT TRUE?
Maybe yes, said SEIU-UHW policy director David Miller. But he doesn’t see that as a bad thing.
“Yeah, we organize workers, that’s absolutely what we do, but we think the outcome of that is for good,” Miller said. “We want to represent all of the workers in the state… we represent workers’ interest in the economy against pretty significant for-profit owners.”
Union president Dave Regan has made aggressive use of ballot propositions as a tool for advancing labor interests. The union has filed dozens of initiatives in California alone, and some did convince hospitals to engage in negotiations.
To the extent that the dialysis initiatives are an organizing tactic, Fairbanks said it’s a bad one.
“What they should continue doing, and what everyone wants them to continue doing, is continue talking to employees, continue meeting them in parking lots, continue doing the visits, continue sending them letters, continue sending them texts,” she said. “But don’t put dialysis patients in harm’s way every two years with these ballot measures that won’t improve patient care.”
THE UNION HAS LOST BADLY TWICE. WHY IS IT TRYING AGAIN TO PUSH THROUGH THE SAME PROPOSAL?
SEIU-UHW said it has listened to feedback and adjusted its approach after each election. Proposition 8 in 2018 would have set a cap on clinic profit margins. In 2020, Proposition 23 would have required a physician to be at a clinic at all times.
This time around, said policy director Miller, there are some important changes.
“There was a critique that there aren’t enough physicians to cover what we’re asking them to do,” Miller said. “So we expanded the number of advanced practitioners who can work in sites. We heard criticism… you move closer to your opposition when you’re trying to get something passed.”
IS THE INDUSTRY STILL TAKING THE MEASURE SERIOUSLY?
Yes. Top contributors to the No on 29 campaign have spent nearly $43 million in this cycle. DaVita is nearing $25 million in contributions, while Fresnius has chipped in almost $12 million.
This story was originally published September 13, 2022 at 5:00 AM.